Sleep and the student experience: A review
Summary: This webpage hosts a review of scientific studies related to sleep and the student experience. Thanks for visiting – please have a read and comment below.
Authors: Eleni Pitsiniaga, Philip J. Heron
Institution: Department of Physical and Environmental Science, University of Toronto Scarborough
Abstract
Current research suggests that sleep deprivation is gradually becoming an international pandemic. Although the negative effects of sleep loss influence people at any point in their life, it may significantly compromise students’ motivation and learning abilities. In this paper, we review studies that demonstrate the correlation between sleep and academic success, focusing on memory retention, alertness, mental health, and physical performance. We propose potential actions for students and university administrators to promote sleep education and support healthy sleeping habits. It is imperative to acknowledge the impact of sleep on the student experience given the influence that a university education has on shaping a student’s future.
Introduction
The student experience of going to university to study for a degree can be a significant life achievement that allows future professionals to expand their knowledge, abilities, and career earnings (Carnevale et al., 2021). Given the importance of this experience, attending university has become a place of high stress to perform in increasingly competitive academic situations (Gillen-O’Neel et al., 2013). As a result, students often sacrifice their sleep (Gillen-O’Neel et al., 2013), leading to a significant prevalence of daytime sleepiness, sleep deprivation, and inconsistent sleep cycles (Hershner & Chervin., 2014).
The student experience is often centered on the need for ‘successful’ Grade Point Average (GPA). A student’s GPA may be influenced by their motivation, character, socioeconomic situation, work ethic, health condition, course load, multitasking abilities, and test-taking skills (Hershner & Chervin, 2014). However, there is evidence to support a link between sleep and GPA, since it has been demonstrated that long sleepers (9 hours) tend to have higher GPAs (average GPA: 3.24) than short sleepers (6 hours) did on average (average GPA: 2.74) (Kelly et al., 2001).
Sleep deprivation (e.g., insufficient sleep to maintain alertness during the day) affects 50% of university students, opposed to 36% of teenagers and adults (Oginska & Pokorski, 2006). Approximately 60% of students report feeling exhausted or burnt out for at least three days of the week (Hershner & Chervin, 2014). While the ideal amount of sleep for a young adult is 8 hours, 71% of undergraduate students reported sleep less than 8 hours per night (Hershner & Chervin, 2014). A typical stereotype about university students is that they barely sleep (Gillen-O’Neel et al., 2013; Acharya et al., 2018), which can compromise academic success (Saghir et al., 2018). The purpose of this paper is to review the consequences of sleep deprivation on psychological, cognitive, and physical functions related to the student experience, and outline the potential impact of sleep education on the lifestyle and academic experience of the student body.
Effects on psychology on mental health
Depression is the most commonly occurring psychiatric disease among undergraduate students in America, impacting 35% of students nationwide (Acharya et al., 2018). Students demonstrating depressive symptoms express sleep disturbances and fail to obtain good quality sleep (Acharya et al., 2018).
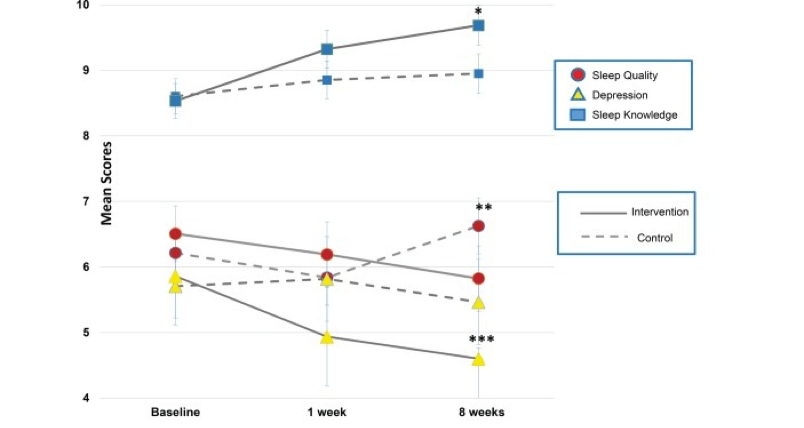
Hershner et al. (2018) examined depression with regards to hours of sleep of university students over the span of 8 weeks by randomly splitting them into two groups. The first group consisted of 295 ‘control’ participants and the second consisted of 254 ‘intervention’ participants; the only difference between groups being that the intervention group was provided with sufficient sleep education that highlighted the risks and benefits of a good night’s sleep. At the end of the 8-week period, participants completed the Patient Health Questionnaire (PHQ-9), where they ranked a list of 9 depressive symptoms on a scale from 0 (not at all) to 3 (nearly every day). Using these scores, they created the following scale to assess the severity of depression: none (0–4), mild (5–9), moderate (10–14), moderately severe (15–19), and severe (20–27). For the intervention group participants, 33% demonstrated significantly better sleep quality, in addition to lower depression scores (Figure 1). Specifically, only 14% of the intervention group expressed symptoms of depression, as opposed to the 36% of the control participants.
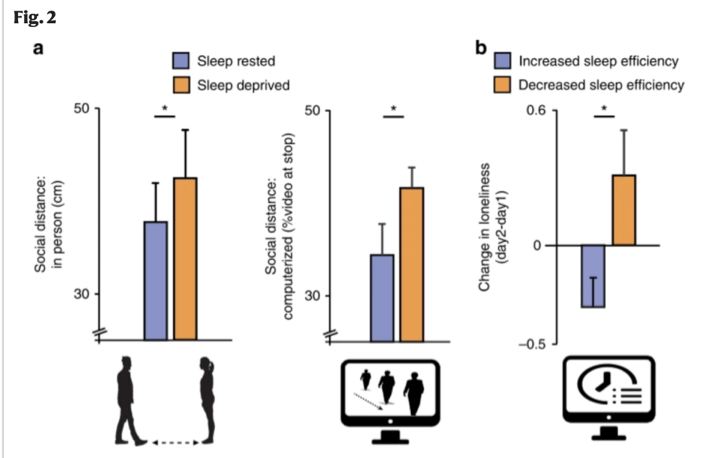
To assess the effects sleep deprivation poses on social withdrawal and loneliness, Simon & Walker (2018) tested 18 healthy adults of ages 18-24 under well-rested conditions and under sleep deprivation. In the first part of this study, they allowed participants to socialize with an experimenter, initially from a 3-meter distance while the experimenter was slowly approaching them. The participants told the experimenters to “stop” when they maintained a comfortable distance, followed by a distance participants found uncomfortable. The space reflecting the uncomfortable distance, demonstrated participant tolerance for social and physical propinquity, as the sleep deprived participants maintained a longer distance from their experimenter (Figure 2). Additionally, the study monitored the participants’ reaction to a recording of a group of individuals approaching them. Using Functional Magnetic Resonance Imaging (fMRI) scans taken during the virtual tests, they observed changes in the brain activity between both conditions, and then called to perform an interview. In this interview, participants were asked a series of questions on various topics. Furthermore, they invited a group of judges independent from the study to review the interview footage and evaluate their socioemotional and energy levels. They concluded that the sleep deprived individuals were less likely to participate in social situations and demonstrated lonelier tendencies (Figure 2).
Chellappa & Araújo, (2007) conducted a similar experiment, this time to investigate the affects sleep deprivation poses on suicidal tendencies. Seventy participants were chosen for this study between the ages of 18 and 65 that demonstrated a major depressive disorder diagnosis. Experimenters were able to diagnose patients through an interview in addition to the Diagnostic and Statistical Manual of Mental Disorders. Suicidal intention was measured using a 19-item list Beck Scale Suicidal Ideation (SSI) where participants rated their suicidal tendencies, followed by an interview by an experimenter (Beck et al., 1979). Significant suicidal intent was indicated by an SSI score of ≥6. Sleep quality was assessed from the Sleep Habits questionnaire (SHQ) to indicate if participants suffered from insomnia or excessive sleepiness (e.g., if participants demonstrated an increased urge to sleep, as well as the propensity to take unwanted naps) . The results of this study demonstrated that insomniac patients had significantly greater SSI ratings (7.39±2.84), as well as significantly higher tendencies for active suicidal ideation, previous suicide attempts, and specific plans for suicide, compared to participants with excessive sleepiness (SSI rating of 3.86±1.73).
Effects on memory retention and alertness
A number of psychological effects, including depression, anxiety, emotional distress, low self-esteem, and behavioral problems, are typically correlated with GPA, with academic success dictating students wellbeing (Dong et al., 2021). A deficient memory would only maximize these unwanted effects due to a reduced capacity to solidify information through studying (Dong et al., 2021). Sleep deprivation influences memory retention, cognitive levels, and overall alertness (Hershner & Chervin, 2014). Recalling back to Hershner et al. (2018), 73% of undergraduates admitted to getting insufficient sleep during weeknights (<7 hour/night) before the experimental sleep intervention. In addition to this, 78% of students claimed that their academic performance was significantly impacted by their fatigue.
Lo et al. (2016) examined the relationship between sleep deprivation and false memory retention by separating 60 healthy university students (average age of 22.10 ± 1.60 years) into three categories: those expressing total sleep deprivation (23 hours of sleep deprivation), partial sleep deprivation (5 hours of sleep), and a control group (8 hours of sleep). The tests were conducted in three phases: event-coding, misinformation, and a memory test. In the first phase (event-coding), students from each group were shown 50 images depicting a crime scene. In the second phase (misinformation), the students were exposed to two narratives, without knowing that the information they were given was contradicting the images. In the third phase (memory test), they were asked to recall the information provided by answering a series of questions and indicating whether they remember that information from the picture, the narrative, or both. The total sleep deprived group demonstrated the highest misinformation retention, while the control showed the least. Additionally, they concluded that the retention of false information increased following several nights of sleep deprivation.
In relation to alertness, sleep deprived drivers are involved in ~33% of road fatalities (AlShareef, 2021). A study conducted by Williamson & Feyer (2000) reported that following a 17 to 19-hour sleep loss period, performance speed on cognitive tests was reduced as much as 50% in participants. This result was lower than participants who had a blood-alcohol content (BAC) of 0.05%. Longer durations of time without sleep (>28 hours) resulted in performance levels comparable to the highest alcohol dose administered to individuals (BAC of 0.1%, 1.25 times higher than the driving BAC limit in Canada). The impact of sleep deprivation on alertness during driving is highlighted in a study conducted by Wahlstrom et al. (2014). This study collected data over the span of three years and involved more than 9,000 students. Wahlstrom et al. (2014) recorded the amount of car crashes that involved student drivers for schools that started at 7:35 AM and 8:30 AM respectively. When schools changed start times from 7:35 AM to 8:55 AM, the occurrence of vehicle accidents involving student drivers decreased by 70% as the young drivers were more alert and conscious behind the wheel. Furthermore, they discovered that the schools that started at 8:30 AM enabled more than 60% of students to achieve minimum eight hours of sleep each school night.
Effects on the body and physiology
In the United States, approximately 9% of all young athletes (3.5 million people) require medical attention for sports-related accidents (Milewski et al., 2014). Sleep loss is known to reduce reaction times, influence mood, and impair cognitive abilities that may render young athletes more susceptible to injury (Philip et al., 2004).
Milewski et al. (2014) reported 205 total injuries from 64 adolescent athletes that participated in a survey to determine the effects of sleep deprivation on injury risk. In this study consisting of 112 participants, 57% had sustained athletic injuries as a result of the lack of sleep; 42 of those athletes had sustained more than one injury in that year. Upon comparing the sleeping habits of the adolescents, 65% of the participants that were injured reported to sleep less than 8 hours per night, as opposed to the 31% who slept more than 8 hours per night. Using this information, Milewski et al. (2014) adapted Figure 3 to demonstrate the relationship between the potential risk of injury and hours of sleep.

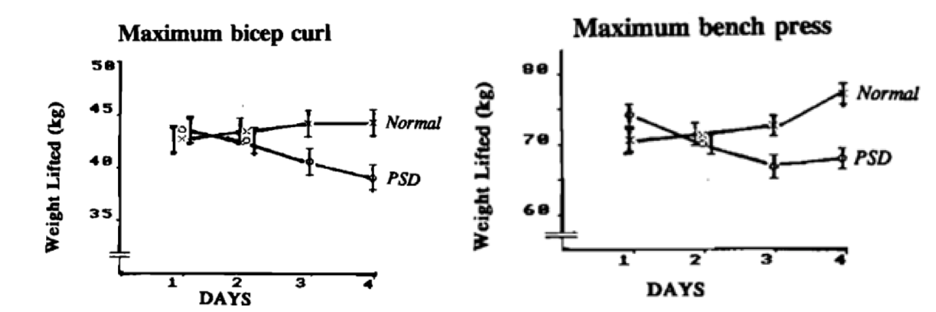
A study conducted by Reilly & Piercy (2007) evaluated the effects sleep loss has on athletic performance. In this study, eight healthy males aged 18-24 years old were subject to 8 (±1) hour periods of sufficient sleep per night in addition to periods of only 3 hours of sleep per night. In both cases, the participants completed heavy weightlifting work-out exercises (bicep curl, bench press, leg press, and deadlift) and were evaluated on their perception of effort and weight lifted. By comparing these two conditions, researchers were able to define an overall 15-20% decline in effort and amount of weight lifted in during the periods of sleep deprivation (Figure 4).
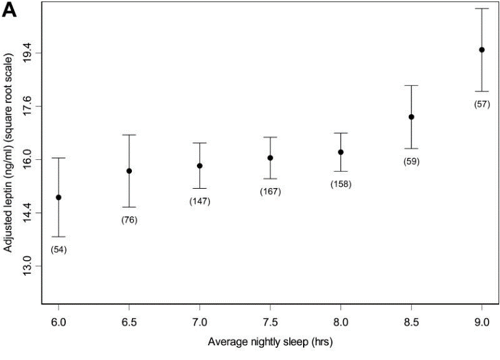
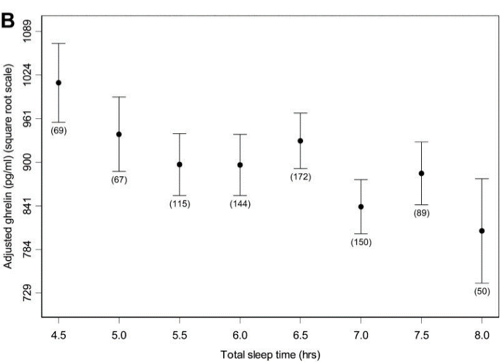
In terms of health, sleep deprivation promotes diabetes and weight gain, as shown in Taheri et al. (2004) through examining the relationship between insufficient sleep and high Body Mass Index (BMI). The study inferred that the two main antagonistic hormones in hunger control, leptin and ghrelin, were important factors in the relationship. Leptin is a hormone that reduces appetite while ghrelin promotes it. As demonstrated by Figure 5, following a restless night of sleep, the expression of ghrelin dominates the expression of leptin, leading to an increased desire in appetite (Taheri et al., 2004).
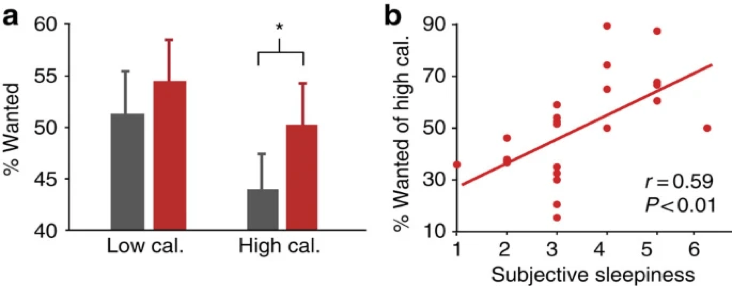
Specifically looking at food choices for the sleep deprived, Greer et al. (2013) assessed the relationship between sleep loss and cravings for high caloric foods. Here, 23 healthy individuals (13 female; age: 20.5±1.8 s.d.; BMI: 23.0±1.8 s.d.) were subjected to a period sufficient sleep (~8.2 hours/night) and a period of sleep deprivation (~24.6 hours awake). Under both conditions, participants were fed a regulated diet that contained enough energy to remain awake. Using a scale of 1-4, where 1 is least desired and 4 is strongly desired, participants were asked to rate a selection of 80 food items with varying caloric compositions. The results of this study suggested that cravings for food with high caloric contents are heavily associated with sleep deprivation (Figure 6).
Discussion
This paper reviews studies that analyze sleep deprivation and its impact on functions related to the student experience (e.g., memory retention, mental health, alertness, athletic performance). A limitation of this review relates to the potential variability of the results of the studies highlighted here and different subject demographics. As an example, results may change if the research was conducted on subjects with a different geographic location, economic status, academic background, and social status. In those studies featuring university students, most did not specify the subjects’ program of study as well as the hours they allocate daily for studying, which may impact the findings.
An area of significance to the student experience where there seems to be no consensus in the scientific literature is the positive or negative impact of naps. Wiegand et al. (1993) claim that there is no significant correlation between naps to increase mood following sleep deprivation. However, Brooks & Lack (2006) and Taub et al. (1976) marked an increase in alertness, task performance, and mood after napping for five to 30 minutes compared to the subjects that did not nap (McDevitt et al., 2018). An area of future work would be to fully understand the impact of naps, which may be important in understanding the student experience.
Fortunately, there are many tips that act as a guideline for students to follow in order to develop a healthier relationship with sleep. These tips include (Choe et al., 2011):
- preferring not to sacrifice their sleep to study,
- developing self-care habits,
- psychological therapy,
- maintaining a consistent sleeping and waking up schedule,
- not exercising at least three hours before expected bedtime,
- avoiding smoking, caffeine, and alcohol before bed,
- and setting up a comfortable bedroom with limited to no light or noise.
Students should also avoid attempting to fall asleep while they are experiencing high stress and should engage in activities such as reading if they are unable to sleep within 30 minutes of going to bed (Choe et al., 2011). It is important to note that in the age where the bedroom, specifically the bed, is a place for sleeping, eating, working, exercising, entertainment, and studying, it is becoming ever more difficult to associate the bed with the place of sleep. As a result, it is vital for students to refrain from performing these activities from their bed and should reserve this space only for sleep and sexual activities (Choe et al., 2011).
University administration also have some responsibility in promoting positive sleep behaviour, alongside student personal responsibility. As an example, course examination should prefer to assign untimed assignment-based exams which test student understanding under different conditions than more traditional timed exams (Fellenz, 2004). In North American universities, final exams often occur shortly after the end of term, leading to a pressure situation of ‘cramming’ to prepare. This often creates a situation where multiple exams need to be studied for, which can promote shorter sleep patterns (Zunhammer et al., 2014) and higher stress (Fejes et al., 2020) – which may ultimately create poor long term retention of information (Walker, 2009). A change to the exam schedule, and/or the application of untimed assignments, could relieve a considerable amount of student stress andmay improve the student experience (Hershner et al. 2018).
Furthermore, typical university-age students (e.g., young adults and teenagers) generally possess a delayed circadian rhythm preference following the physiology of “night owls” (Jenni & Carskadon, 2007). The circadian rhythm acts as an internal clock that controls hormone production and sleep/wake cycles. “Night owls” refers to individuals who are more productive in the evening-night hours rather than in the morning. They tend to sleep and wake up later compared to “morning larks” (Schoedel et al., 2020). Young people that are more physically developed than children typically prefer later bedtimes, may have a reduced homeostatic sleep drive, and feel more productive at night (Hershner & Chervin, 2014). An adolescent’s circadian period is 24.3 hours, which is longer than the average adult (24.1 hours), allowing for a bedtime later in the day (Crowley et al., 2007). Another suggestion to university administration would be to change early morning class start times, which could have an impact on student mental health (Wahlstron, 2002).
A further practical example for university administration is for Wellness centers to provide students with sleep education resources, in addition to sleep experts and therapists that will help undergraduates overcome sleep depriving tendencies. This can be further achieved by implementing courses and regular seminars about the importance of sleep and how to maintain a healthy relationship with sleep. For this review paper, we provide example of posters to be distributed by university wellness centers regarding the impact of sleep on the student experience (Figure 7 and supplementary material).
Conclusion
Recent studies indicate that we are going through a potential global sleep-loss epidemic (Chattu et al., 2018). The impact of lack of sleep can propagate through all stages of life. However, the impact of sleep on the student experience can be significant. In this review paper, we highlight studies related to sleep and key aspect of student life, namely memory retention, alertness, mental health and athletic performance. We outline practical steps that could be taken by students and university administrators to help promote healthy sleep practices. Given the importance of sleep on wellbeing (e.g., Chellappa and Araújo, 2007) and knowing the impact that a university can have on the future of a student (e.g., increased career earnings, Carnevale et al., 2021), it is vital that careful attention be paid to the role of sleep in the student experience (Chatu et al., 2018).

References
Acharya, L., Jin, L., & Collins, W. (2018). College life is stressful today – Emerging stressors and depressive symptoms in college students. J Am Coll Health. 66(7):655-664. https://doi.org/10.1080/07448481.2018.1451869
AlShareef, S. M. (2021). Excessive daytime sleepiness and associations with sleep-related motor vehicle accidents: results from a nationwide survey. Sleep & breathing = Schlaf & Atmung, 25(3), 1671-1676. https://doi.org/10.1007/s11325-020-02260-5
Beck, A. T., Kovacs, M., & Weissman, A. (1979). Assessment of suicidal intention: the Scale for Suicide Ideation. Journal of consulting and clinical psychology, 47(2), 343–352. https://doi.org/10.1037//0022-006x.47.2.343
Carnevale, A. P., Cheah, B., & Wenzinger, E. (2021). The College Payo : More EducationDoesn’t Always Mean More Earnings. Washington,DC: Georgetown University Center on Educationand the Workforce. cew.georgetown.edu/collegepayo 2021.
Chandler, Q. (2019). The negative stereotypes about mental health, and African-American College students’ willingness to seek counseling. Global Journal of Psychology Research New Trends and Issues, 9(2), 32-42. hhtps://doi.org/10.18844/gjpr.v9i2.4208
Chattu, V. K., Manzar, M. D., Kumary, S., Burman, D., Spence, D. W., & Pandi-Perumal, S. R. (2018). The Global Problem of Insufficient Sleep and Its Serious Public Health Implications. Healthcare (Basel, Switzerland), 7(1), 1. https://doi.org/10.3390/healthcare7010001
Chellappa, S. L., & Araújo, J. F. (2007). Sleep disorders and suicidal ideation in patients with depressive disorder. Psychiatry research, 153(2), 131–136. https://doi.org/10.1016/j.psychres.2006.05.007
Crowley SJ, Acebo C, Carskadon MA. Sleep, circadian rhythms, and delayed phase in adolescence. Sleep Med. 2007;8(6):602–612
Dong, X., Yang, K., Zhang, R., & Lv, Y. (2021). The Mental Health and Grade Point Average among College Students from Lower Socioeconomic Status Based on Healthcare Data Analysis. Journal of healthcare engineering, 2021, 2378202. https://doi.org/10.1155/2021/2378202
Fejes, I., Ábrahám, G., & Légrády, P. (2020). The effect of an exam period as a stress situation on baroreflex sensitivity among healthy university students, Blood Pressure, 29:3, 175-181, https://doi.org/10.1080/08037051.2019.1710108
Fellenz, M. R. (2004). Using assessment to support higher level learning: the multiple choice item development assignment, Assessment & Evaluation in Higher Education, 29:6, 703-719. https://doi.org/10.1080/0260293042000227245
Gillen-O’Neel, C., Huynh, V. W., & Fuligni, A. J. (2013). To Study or to Sleep? The Academic Costs of Extra Studying at the Expense of Sleep. Child Development, 84(1), 133–142. https://doi.org/10.1111/j.1467-8624.2012.01834.x
Greer, S. M., Goldstein, A. N., & Walker, M. P. (2013). The impact of sleep deprivation on food desire in the human brain. Nature communications, 4, 2259. https://doi.org/10.1038/ncomms3259
Hershner, S. D., & Chervin, R. D. (2014). Causes and consequences of sleepiness among college students. Nature and science of sleep, 6, 73–84. https://doi.org/10.2147/NSS.S62907
Hershner, S., & O’Brien, L. M. (2018). The Impact of a Randomized Sleep Education Intervention for College Students. Journal of clinical sleep medicine, 14(3), 337–347. https://doi.org/10.5664/jcsm.6974
Jenni, O. G., & Carskadon, M. A., (2007). Sleep behavior and sleep regulation from infancy through adolescence: normative aspects. Sleep Med Clin, 2(3), 321–329. https://doi.org/10.1016/j.jsmc.2012.06.002
Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: validity of a brief depression severity Measure. Journal of general internal medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Lo, J.C., Chong, P.L.H., Ganesan, S., Leong, R.L.F., & Chee, M.W.L. (2016). Sleep deprivation increases formation of false memory. J Sleep Res, 25: 673-682. https://doi.org/10.1111/jsr.12436
McDevitt, E. A., Sattari, N., Duggan, K. A., Cellini, N., Whitehurst, L. N., Perera, C., Reihanabad, N., Granados, S., Hernandez, L., & Mednick, S. C. (2018). The impact of frequent napping and nap practice on sleep-dependent memory in humans. Scientific reports, 8(1), 15053. https://doi.org/10.1038/s41598-018-33209-0
Milewski, M. D., Skaggs, D. L., Bishop, G. A., Pace, J. L., Ibrahim, D. A., Wren, T. A. L., & Barzdukas, A. (2014) Chronic Lack of Sleep is Associated With Increased Sports Injuries in Adolescent Athletes, Journal of Pediatric Orthopaedics 34(2), 129-133. https://doi.org/10.1097/BPO.0000000000000151
Oginska, H., & Pokorski, J. (2006). Fatigue and mood correlates of sleep length in three age-social groups: School children, students, and employees. Chronobiology international, 23(6), 1317– 1328. https://doi.org/10.1080/07420520601089349
Philip, P., Taillard, J., Sagaspe, P., Valtat, C., Sanchez-Ortuno, M., Moore, N., Charles, A., & Bioulac, B. (2004). Age, performance and sleep deprivation. Journal of sleep research, 13(2), 105–110. https://doi.org/10.1111/j.1365-2869.2004.00399.x
Saghir, Z., Syeda, J. N., Muhammad, A. S., & Balla Abdalla, T. H. (2018). The Amygdala, Sleep Debt, Sleep Deprivation, and the Emotion of Anger: A Possible Connection?. Cureus, 10(7), e2912.
https://doi.org/10.7759/cureus.2912
Simon, B.E., & Walker, M.P. (2018). Sleep loss causes social withdrawal and loneliness. Nat Commun 9, 3146. https://doi.org/10.1038/s41467-018-05377-0
Schoedel, R., Pargent, F., Au, Q., Völkel, S. T., Schuwerk, T., Bühner, M., & Stachl, C. (2020). To Challenge the Morning Lark and the Night Owl: Using Smartphone Sensing Data to Investigate Day–Night Behaviour Patterns. European Journal of Personality, 34(5), 733–752. https://doi.org/10.1002/per.2258
Taheri, S., Lin, L., Austin, D., Young, T., & Mignot, E. (2004). Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS medicine, 1(3), e62. https://doi.org/10.1371/journal.pmed.0010062
Reilly, T., & Piercy, M. (2007). The effect of partial sleep deprivation on weight-lifting performance, Ergonomics, 37:1, 107-115. https://doi.org/10.1080/00140139408963628
Wahlstrom, K. (2002), Changing times: Findings from the first longitudinal study of later high school start times. NASSP Bulletin, 83, 633, https://doi.org/10.1177/019263650208663302
Wahlstrom, K; Dretzke, B; Gordon, M; Peterson, K; Edwards, K; Gdula, J. (2014). Examining the Impact of Later High School Start Times on the Health and Academic Performance of High School Students: A Multi-Site Study. Retrieved from the University of Minnesota Digital Conservancy, https://hdl.handle.net/11299/162769.
Walker M. P. (2009). The role of slow wave sleep in memory processing. Journal of clinical sleep medicine: JCSM: official publication of the American Academy of Sleep Medicine, 5(2 Suppl),S20–S26.
Wiegand, M., Riemann, D., Schreiber, W., Lauer, C. J., & Berger, M. (1993). Effect of morning and afternoon naps on mood after total sleep deprivation in patients with major depression. Biological Psychiatry, 33(6), 467–476. https://doi.org/10.1016/0006-3223(93)90175-D
Williamson, A. M., & Feyer, A. M. (2000). Moderate sleep deprivation produces impairments in cognitive and motor performance equivalent to legally prescribed levels of alcohol intoxication. Occupational and environmental medicine, 57(10), 649–655. https://doi.org/10.1136/oem.57.10.649
Zunhammer, M., Eichhammer, P., & Busch, V. (2014). Sleep quality during exam stress: the role of alcohol, caffeine and nicotine. PloS one, 9(10), e109490. https://doi.org/10.1371/journal.pone.0109490